Story Highlight
– Cross-sex hormones help align physical appearance with gender.
– NHS decision deemed overdue by legal representatives.
– Concerns raised over private sector treatment safety.
– Call for immediate ban on private sector prescriptions.
– Claimant highlights inconsistency in treatment across sectors.
Full Story
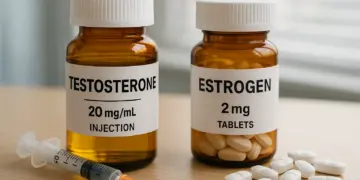
The recent discourse surrounding cross-sex hormones has intensified following significant decisions made by healthcare authorities. Cross-sex hormones, including testosterone and oestrogen, are employed by individuals seeking to modify their physical characteristics to better reflect their gender identity. This treatment aims to facilitate changes such as breast development or increased body hair. Crucially, these hormones differ from puberty blockers, which temporarily halt the natural hormone production that facilitates the transition from childhood to adulthood.
The debate has garnered attention from various stakeholders, including legal representatives and activists advocating for the rights and safety of minors. Paul Conrathe, a partner at Conrathe Gardner LLP, is representing individuals who have raised concerns regarding the National Health Service (NHS) and its policies related to hormone treatment. In a statement to the press, Conrathe characterised the recent NHS decision as “overdue,” highlighting the potential risks that adolescents face if they seek treatment outside the public health system.
He expressed concern that while the NHS parameters provide crucial safeguards for teenagers in its care, they simultaneously create a gap that may expose others to unregulated treatments offered by private providers. Conrathe emphasized that allowing private clinics to continue prescribing these hormones would be “irrational” and represent a failure in the responsibilities shouldered by the Secretary of State for Health.
In response to the situation, Conrathe has formally written to the Secretary, urging immediate action to impose a ban on such treatments within the private healthcare sector. He warned that without prompt intervention, his group is prepared to initiate legal proceedings in the High Court. This stance has raised significant dialogue around the complexities of regulating gender-affirming care in both public and private healthcare systems.
One of the individuals affected by these policies is Keira Bell, who underwent hormone treatment at the Tavistock clinic. Reflecting on her experience, Bell stated that it is “completely illogical to ban these drugs for children in one sector and not the other.” Her comments resonate with a broader concern that disparate regulations across healthcare settings could lead to inconsistencies in care and protection for vulnerable patients.
The ongoing discussion brings into focus the ethical considerations surrounding gender-affirming treatments, particularly for minors. Advocates for stringent regulations argue that young people may not fully understand the permanent effects of such treatments and could be making decisions with lifelong consequences. Critics of the current framework, however, advocate for a model that respects the autonomy of young individuals to make informed choices about their identities and bodies.
The context of these debates is further complicated by differing perspectives on what constitutes informed consent, particularly for adolescents. Many experts urge for more comprehensive guidelines to ensure that young people seeking such treatments are adequately informed about the options available to them and the potential risks involved. This includes the importance of thorough psychological assessment and counselling beforehand, aimed at guiding individuals through the complexities of their choices.
This polarised dialogue is unfolding amidst wider societal changes regarding the understanding of gender and its expression. As awareness grows, so too does the pressure on healthcare systems to evolve in response to the needs of diverse populations. The calls for action from figures like Conrathe and Bell reflect a sense of urgency felt by many who believe that a regulatory framework is necessary to ensure safety and ethical treatment standards.
In light of these developments, there has been an increasing demand for more empirical research into the long-term effects of cross-sex hormones and puberty blockers. The need for robust data is seen as essential for informing policy decisions and healthcare practices, ensuring that they are not just reactive, but guided by scientific evidence and best practices.
While the conversation continues, it is evident that the landscape of gender-affirming care is not only a medical issue but also deeply intertwined with social, ethical, and political dimensions. As stakeholders—from healthcare professionals to legal advocates—grapple with these questions, the implications for young people’s rights and health outcomes remain paramount.
The outcomes of these discussions will likely have significant repercussions for future policies surrounding gender-affirming care. This complex interplay of factors will require ongoing scrutiny and engagement from all sides to navigate the best course forward, ensuring that the wellbeing of young individuals remains at the forefront of any legislative or healthcare considerations moving ahead.
Our Thoughts
The article highlights concerns regarding the prescription of cross-sex hormones to teenagers, particularly in the private sector, raising safety and regulatory issues. To prevent incidents like this, a more robust regulatory framework should be established to ensure uniform treatment practices across both NHS and private sectors, in line with the Health and Safety at Work Act 1974, which mandates safe practices in healthcare.
Key safety lessons include the need for improved risk assessments and stringent guidelines for prescribing hormone treatments. Ensuring informed consent processes that adequately communicate the potential risks and benefits is essential.
Relevant regulations, such as the Misuse of Drugs Act 1971, may also have implications for the prescribing of these hormones, calling for clearer guidelines on their administration. The failure to provide standardized protocols could leave teenagers exposed to unregulated treatment options.
Preventive measures could include mandatory oversight of private clinics and the establishment of a regulatory body to monitor the administration of hormone therapies, ensuring that all practices adhere to the same safety standards as those within the NHS.