Story Highlight
– Injectable peptides for beauty pose significant health risks.
– TikTok influences demand for unregulated injectable treatments.
– Many peptides lack safety data for human use.
– Users become unregulated test subjects for health products.
– Incidents in the US highlight dangers of peptide injections.
Full Story
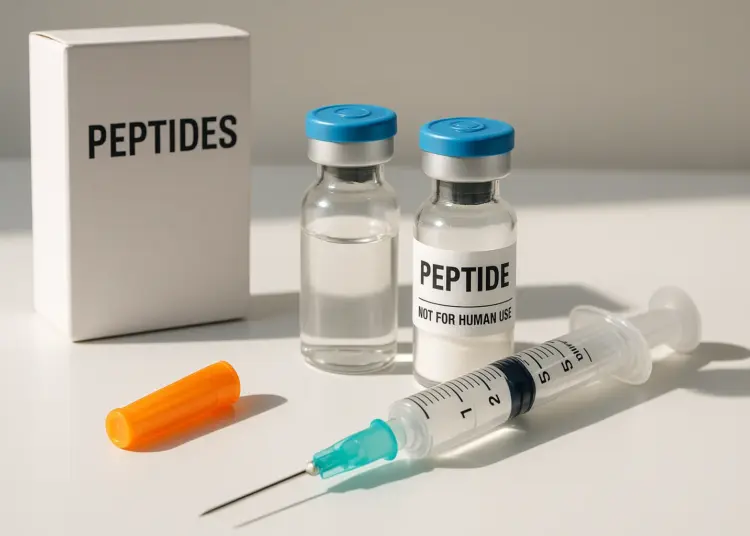
The growing interest in beauty enhancement among social media users has paved the way for an alarming trend: the injection of peptides for cosmetic purposes. While the term “peptides” is frequently encountered in skincare products, distinguishing between topical and injectable peptides can be confusing. While the former—like copper and argireline—have been widely used in serums and lotions and are generally considered safe, a more hazardous practice has emerged involving the injection of unregulated peptides that claim to promote various beauty benefits.
Injectable peptides are primarily sought after for claims that they can enhance skin appearance, improve hair quality, and contribute to overall wellness. However, many of these substances are not approved for human use in the UK, raising serious safety concerns. The injections typically consist of short chains of amino acids that occur naturally in the body. They are administered subcutaneously, often around the abdomen, with the aim of stimulating collagen synthesis and deeper tissue repair. Despite their touted benefits, these substances carry potential risks, and the absence of extensive research raises profound questions about their safety.
The rise of injectable peptides is part of a larger movement towards biohacking—a trend that encourages individuals to take control of their health through unconventional methods, often at the expense of safety. This movement has been linked to a culture of ‘looksmaxxing’, where individuals strive for their ideal appearance by any means necessary. Influencers on social media have significantly contributed to the popularity of these peptides, often sharing their unique combinations—referred to as ‘stacks’—in hopes that followers will emulate their results.
Dr. Ben Taylor-Davies, co-founder of The Stockbridge Clinic, voices strong concerns over this practice. He emphasizes the importance of regulation within the beauty industry, stating, “While it’s great to see people taking a proactive approach to their health, the increased use of injectable peptides is very concerning.” According to Dr. Taylor-Davies, established medical treatments undergo rigorous scientific scrutiny, a distinction that injectable peptides lack. The long-term health implications of these unregulated substances remain largely unknown, suggesting that users may essentially be subjecting themselves to experimental treatments.
Prominent examples of injectable peptides include GHK-Cu and BPC-157, both of which have yet to be validated through robust clinical trials. As beauty enthusiasts experiment with these substances, many are effectively acting as test subjects, potentially risking their health in the process. The usage of peptides, especially for aesthetic purposes, has drawn comparison to medications such as GLP-1 receptor agonists—like Ozempic and Mounjaro—which have been characterized by their focus on weight loss and metabolic regulation. However, unlike these approved drugs, the safety profile of many injectable peptides remains largely uncharted territory.
Recent incidents highlight the dangerous potential of these cosmetic injections. In an illustrative case from early 2026, a physician and pharmacist in the United States faced fines after administering peptide injections at an anti-aging conference, an event that led to serious complications for some participants. The repercussions included hospitalisation and the need for mechanical ventilation. Although the UK has not reported similar serious cases thus far, experts warn that the trend of peptide injections could soon cross the Atlantic, especially as their popularity continues to surge in wellness circles.
In fact, reports indicate that tech industry employees in San Francisco have been engaging in ‘peptide raves’, events where participants are instructed on how to self-administer these injections in casual and often unsafe settings. Such gatherings epitomize a growing acceptance of risky beauty practices, where the allure of quick results usurps the need for caution and medical oversight.
The debate surrounding injectable peptides also touches on broader themes of beauty standards and societal pressures. The desire to achieve the ‘perfect’ look often drives individuals towards methods that promise rapid transformations, reinforcing cycle after cycle of risk-taking behavior. While the quest for beauty is a long-standing narrative, the means by which individuals seek it—especially in an unregulated environment—could have dire consequences.
In conclusion, while the beauty industry continues to evolve with innovative practices, the proliferation of injectable peptides raises significant health concerns that cannot be ignored. As individuals explore these new frontiers in self-enhancement, the pressing need for thorough research and stringent regulation becomes ever clearer. Until the safety and efficacy of these products are established through controlled studies, the advice remains sound: caution is paramount, and the pursuit of health and beauty should not come at the cost of one’s well-being.
Our Thoughts
The rise of injectable peptides for beauty purposes poses significant health risks, particularly due to their unregulated status in the UK. To avoid potential health crises linked to these practices, clearer regulatory frameworks should be established to control the sale and administration of injectable substances. According to the Health and Safety at Work Act 1974, employers must ensure the health and safety of their workers, which extends to anyone administering treatments. Without appropriate approvals and clinical testing, these practices violate the Medicines Act 1968, which mandates that medicines must be safe, effective, and of good quality.
Key safety lessons include the importance of preventing unapproved medical practices by promoting awareness around the risks of self-administered injections and ensuring that individuals consult qualified health professionals. Greater public education campaigns could help mitigate the trend. Developing stringent guidelines for cosmetic injectables could help prevent similar incidents in the future, ensuring that only safe, clinically tested products are used for beauty treatments. Enhanced monitoring and enforcement of regulations governing medical substances will be essential in protecting public health.