Story Highlight
– NHS England reviews private clinic agreements for gender care.
– Concern over patient safety with unregulated providers.
– GPs advised against prescribing for under-18s via private clinics.
– Calls for timely access to gender-affirming care criticized.
– Evidence reviews on hormone treatments are forthcoming.
Full Story
NHS England is evaluating its collaborations with private clinics regarding the provision of gender-affirming healthcare for adults, as raised in a recent update. The public health authority has expressed concerns regarding the safety of shared care agreements that allow general practitioners (GPs) to prescribe hormone treatments sourced from these private providers.
In the UK, GPs can create “shared care agreements” with both public and private healthcare entities to facilitate the prescription of various medications. This arrangement typically involves clinics supplying GPs with advice on appropriate prescribing practices.
A report released last week highlights NHS England’s stance that these private services may pose a potential risk to patient safety across different age groups. The agency suggested that GPs should abstain from offering support for gender-affirming treatments for transgender individuals under the age of 18 through these agreements. The guidance advises GPs to recommend that patients and their guardians avoid medications obtained from unregulated sources.
Among the private providers identified for potential exclusion from these agreements are prominent clinics such as GenderGP and Anne Trans Healthcare Limited, both of which are well-known in the UK for offering transgender healthcare services.
While the report specifically addresses the concerns surrounding minors, NHS England has indicated plans to assess whether similar recommendations should be extended to adult care in the future. The NHS report articulates that “in recognition that unregulated healthcare services pose a potential risk to patient safety across all age ranges,” it will revisit how adults who source medications outside NHS-approved gender dysphoria services are managed. This review is part of broader efforts to formulate a new clinical commissioning policy regarding prescribed hormones, expected to be implemented by the 2025/26 period.
Previous leaked guidance from NHS England last April hinted that officials were contemplating the discontinuation of shared care agreements with non-NHS-approved clinics for patients under 18. However, recent actions have seen many GPs increasingly halting the prescriptions of hormone treatments for transgender patients, citing perceived deficiencies in their expertise as a contributing factor.
Nonetheless, GPs have been willing to prescribe hormones to cisgender adults and administer puberty blockers to minors for other medical conditions such as precocious puberty and menopause.
Critics have voiced strong objections to NHS England’s approach towards transgender healthcare. Tammy Hymas, policy lead for TransActual, has spoken out against the decision to reassess shared care agreements without addressing the difficulties faced by NHS gender identity clinics. Hymas highlighted that many individuals are being compelled to seek gender-affirming care from private clinics due to lengthy waiting times for initial appointments at gender clinics, with some reportedly waiting upwards of eight years.
“By implementing a system that permits access to gender-affirming care based on informed consent, the NHS could significantly alleviate these waiting lists,” Hymas stated, pointing to longstanding evidence and international best practices that support such an approach. “Instead, the current system views transgender individuals as if they are experiencing a psychiatric condition requiring extensive evaluations to receive care. Everyone deserves bodily autonomy, and this should equally apply to access to hormone treatments for transgender people.”
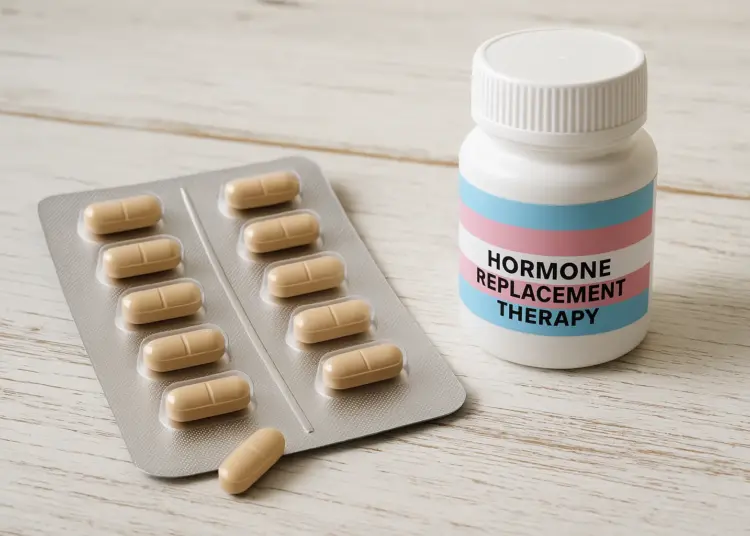
In tandem with the review of shared care agreements, the NHS announced it would be evaluating the effectiveness of hormone replacement therapy (HRT) for transgender adults. This announcement aligns with decisions recently made regarding the prescription of masculinising and feminising hormones for 16 to 17-year-olds.
These measures form part of a larger initiative—an Equality and Health Inequalities Impact Assessment (EHIA)—that includes ten reviews related to various aspects of transgender healthcare, aiming to implement recommendations made by Dr Hilary Cass in 2024.
Gender Plus, currently the only regulated private provider of transgender healthcare in the UK to hold an ‘Outstanding’ rating from the Care Quality Commission (CQC), expressed disappointment in NHS England’s recent actions. The clinic’s representatives argued that the public health authority’s interpretation of the evidence surrounding gender-affirming care diverges from the consensus established by reputable medical institutions worldwide.
Professor James Palmer, NHS England’s national medical director for specialised services, responded to concerns by stating that the forthcoming evidence reviews would shed light on whether changes to NHS approaches regarding transgender healthcare are warranted. He noted, “The NHS has exercised extreme caution when considering starting people on this treatment.” Furthermore, he mentioned that new referrals for this treatment for 16 to 17-year-olds have been paused while current cases will continue but will require individual reviews with clinical teams.
As discussions continue, the current landscape of gender-affirming care in the UK remains complex, with various stakeholders advocating for better access and improved protocols for transgender individuals seeking essential healthcare services.
Our Thoughts
The situation regarding shared care agreements between NHS GPs and private clinics for gender-affirming care presents several areas for improvement, particularly in risk management and patient safety. To prevent potential issues, NHS England could enforce stricter guidelines on the qualifications and regulations governing private clinics, aligning with the Health and Social Care Act 2008 and the Care Quality Commission’s (CQC) standards.
Additionally, a comprehensive training program for GPs about gender-affirming care would enhance their capacity to make informed decisions, thus minimizing abrupt prescription cancellations. Transparent communication should be established to address the logistical challenges in accessing NHS services, potentially reducing the reliance on unregulated providers.
Furthermore, the existing pressures leading patients to seek care outside NHS frameworks should be urgently addressed, aligning with the Management of Health and Safety at Work Regulations 1999, ensuring a safe and effective response to patient needs.
In summary, strengthening regulatory oversight, enhancing GP training, and improving access to NHS services are key measures to avoid similar incidents and uphold patient safety.